At its simplest level, dental billing is the process of getting a dental practice paid for the services provided to patients. But if you’ve ever stepped foot inside a busy front office, you know it’s anything but “simple.” It is the heartbeat of a practice’s financial health.
Dental billing is a specialized branch of healthcare administration that involves a complex dance between the dental office, the patient, and the insurance company (the payer). It starts the moment a patient calls to schedule an appointment and doesn’t end until the balance on their account reaches zero.
It encompasses:
-
Insurance Verification: Ensuring the patient’s plan is active and covers the intended procedure.
-
Claim Submission: Translating clinical notes into standardized codes (CDT codes) and sending them to the carrier.
-
Payment Posting: Accurately recording payments from both insurance and patients.
-
Accounts Receivable (AR) Management: Chasing down those “stuck” claims that haven’t been paid within 30 days.
Without an efficient billing system, a dental practice is essentially a high-end charity. You provide world-class clinical care, but if the paperwork isn’t perfect, the revenue stays locked behind a wall of insurance bureaucracy.
Why is Dental Billing Important?
You might be the most skilled clinician in the state, but if your billing is leaking revenue, your practice won’t survive to help the next patient.
The importance of dental billing can be broken down into three main pillars:
-
Cash Flow Sustainability: Insurance companies are in the business of keeping their money; dental billers are in the business of getting it back. Consistent, accurate billing ensures a steady stream of income to cover overhead, payroll, and the latest dental technology.
-
Patient Trust: There is nothing that ruins a patient relationship faster than a surprise bill or a claim that was denied because the office forgot to send a simple X-ray. Clear, professional billing creates transparency and builds long-term loyalty.
-
Compliance and Legal Protection: The world of dental coding is highly regulated. Proper billing practices protect you from audits and “gray area” mistakes that could lead to heavy fines or legal trouble.
In short, billing isn’t just “back-office work”—it is the engine that allows the clinical side of the practice to exist.
Is Dental Billing Hard?
If you ask a seasoned professional, they’ll tell you: It’s not just hard; it’s an art form.
Why is it considered difficult? Unlike medical billing, which has been highly standardized for decades, dental billing relies heavily on “clinical necessity” and specific radiographic evidence.
-
The “Proof” Factor: You can’t just say a patient needs a crown. You have to prove it with X-rays, intraoral photos, and detailed narratives.
-
The PPO Maze: Every insurance provider has different rules. Some cover a procedure twice a year; others cover it once every six months. If you miss that nuance, the claim is denied.
-
Constant Updates: Every year, the American Dental Association (ADA) updates the CDT (Current Dental Terminology) codes. Keeping up with what’s deleted, what’s new, and what’s revised is a full-time job.
For a general office manager who is also answering phones and greeting patients, dental billing is incredibly difficult. For a dedicated specialist, it is a strategic game of precision. This is why many practices find that trying to do it “on the side” leads to thousands of dollars in “uncollectible” revenue every single month.
What is the Role of AI in Dental Billing?
As we move through 2026, Artificial Intelligence has shifted from a “futuristic luxury” to a “virtual coworker.” In the context of Guardian Dental Billing, AI isn’t here to replace the human touch—it’s here to make it superhuman.
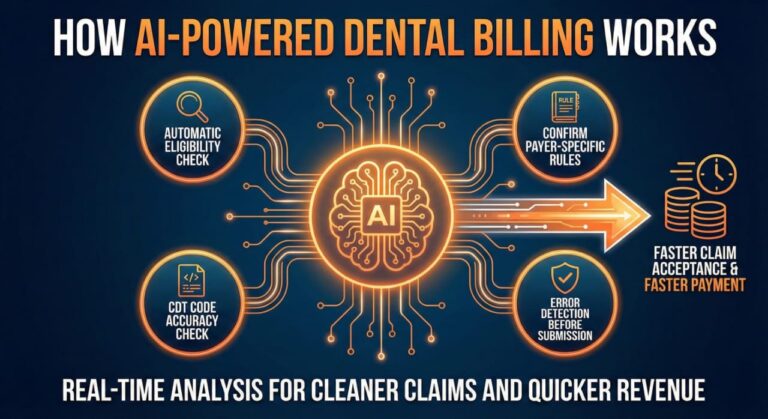
AI’s role today is primarily focused on predictive accuracy and automation of the mundane.
-
Predictive Claim Scrubbing: AI algorithms now scan claims before they are sent, comparing them against millions of successful historical claims. If an X-ray is too blurry or a narrative lacks a specific keyword that a carrier like Delta or MetLife requires, the AI flags it instantly.
-
Real-time Insurance Verification: Gone are the days of staff sitting on hold for 45 minutes. Modern AI “bots” can log into payer portals 24/7 to verify benefits, remaining maximums, and frequency limitations before the patient even walks through the door.
-
Radiographic Analysis: Emerging AI tools can now highlight bone loss or caries on digital X-rays with near-perfect accuracy. For a biller, this provides the “objective proof” needed to attach to a claim, making denials for “lack of clinical necessity” much rarer.
While AI handles the high-volume data, the human expert—the “Guardian”—handles the strategy. AI can flag a denial, but a human understands how to pick up the phone and negotiate with a claims adjuster to get it overturned.
What’s the Difference Between Medical and Dental Billing?
This is where many practices lose thousands of dollars in “hidden” revenue. If you treat dental billing like medical billing, you are playing the right game with the wrong rulebook.
The fundamental difference comes down to Diagnosis vs. Procedure.

In dental billing, you are typically working within a very small bucket of money (the patient’s annual maximum). In medical billing, there is no “annual maximum” in the same sense, but the documentation required to prove medical necessity is significantly more rigorous.
The “Crossover” Opportunity: In 2026, savvy practices are increasingly billing dental procedures—like sleep apnea appliances, TMJ treatments, or bone grafts after trauma—to medical insurance. This preserves the patient’s limited dental benefits for routine care while tapping into their more robust medical coverage. If your billing team doesn’t understand this distinction, you are quite literally giving money back to the insurance companies.
Why Specialization Matters
Because these two systems operate on different software (Dentrix/Eaglesoft for dental vs. Epic/Kareo for medical) and different legal frameworks, you cannot expect a generalist to master both. This is why specialized RCM (Revenue Cycle Management) has become the gold standard. A specialist knows when a case is “just a tooth” and when it’s a “medical condition manifesting in the mouth.”
What Do You Do in Dental Billing?
If you walk into a high-performing dental office, you won’t see the billing team just “typing data.” You’ll see a team of detectives and negotiators. The life of a dental biller is a constant loop of high-stakes verification and precise follow-up.
It is a systematic workflow that, when executed correctly, moves money from an insurance payer’s vault into the practice’s bank account. Here is the typical day-to-day breakdown of a revenue cycle manager:
-
Pre-Appointment Verification (The “Clean Start”): 48 to 72 hours before a patient sits in the chair, a biller verifies eligibility. Is the plan active? Are there frequency limitations (e.g., has the patient already had a cleaning at another office this year)? If you don’t catch a lapse in coverage here, you are often looking at a “Write-Off” later.
-
The Narrative & Clinical Attachments: Insurance companies rarely pay for a crown or periodontal scaling just because you asked. They need evidence. The biller must act as a clinical bridge, ensuring that X-rays, periodontal charts, and narrative explanations (the “why”) are attached to the claim before it hits the payer’s desk.
-
Denial Management (The “Fight”): This is where the real work happens. When a claim comes back with a “denial code,” a great biller doesn’t just give up. They analyze why—was it a coding error? A missing signature? A lack of medical necessity? They then draft appeals, re-submit, and—most importantly—follow up via phone or portal until the claim is paid.
-
Payment Posting & Reconciliation: This is the audit phase. Every dollar that arrives via EOB (Explanation of Benefits) or ERA (Electronic Remittance Advice) must be balanced against the patient’s ledger. If the numbers don’t match, the biller investigates the discrepancy.
Interested in Dental Billing Jobs?
The demand for skilled dental billers—specifically those who understand the nuance of RCM (Revenue Cycle Management)—is at an all-time high. Because practices are becoming larger (moving toward DSO or group practice models), the need for specialized, remote-capable billing talent is booming.
If you are looking to enter this field, or if you are looking to scale your own agency, here is what separates a “data entry clerk” from a “revenue growth partner”:
-
The “CDT Decoder” Mindset: You can’t just rely on software to tell you which code to use. You need an intuitive understanding of the CDT code set and, more importantly, the clinical context behind the procedure.
-
Persistence over Personality: You will spend a lot of time on hold with insurance companies. The best billers have the patience of a saint and the tenacity of a bulldog. They don’t accept the first “no” from a claims adjuster.
-
Software Fluency: Mastery of platforms like Open Dental, Dentrix, Eaglesoft, or Curve is your currency. The faster you can navigate these systems, the more efficient you are.
-
Analytical Capability: The future of this job isn’t just filing claims; it’s reporting. A practice owner wants to know: What is my AR aging report? What is my net collection rate? Where are we losing money? If you can provide these answers, you aren’t just an employee; you are a consultant.
For those in the industry, this career path is unique. It offers a rare blend of stability, remote-work flexibility, and high-level financial problem solving. It’s an ideal field for anyone who enjoys puzzles and wants to have a tangible impact on a business’s growth.
The momentum is building. We’ve established the foundation, the technology, and the day-to-day operations. Now, we move into the “Masterclass” section: the specific tactics for 2026, the complexity of coding, and how a partnership with Guardian Dental Billing turns a struggling back office into a high-performance revenue engine.
Strategy, Mastery, and The Guardian Advantage
What is Dental Coding?
If billing is the vehicle, coding is the fuel. In the dental world, we use the CDT (Current Dental Terminology) code set. These codes are managed by the American Dental Association (ADA) and are updated every single year to reflect new technologies and clinical procedures.
As of 2026, coding has become more granular than ever. For example:
-
Diagnostic Precision: New codes for point-of-care saliva testing and comprehensive cracked tooth testing allow dentists to be compensated for the advanced diagnostics they are already performing.
-
Maintenance & Prevention: There are now specific codes for cleaning and inspecting occlusal guards and specialized debridement for implants.
-
Anesthesia & Restorative: Significant shifts in how deep sedation is documented and the removal of “lesion depth” requirements for posterior composites mean your templates must be updated to avoid instant “outdated code” denials.
The biggest mistake a practice makes? Using “placeholder” codes because they are unsure. In 2026, insurance AI will flag these “generic” submissions for manual review, delaying your payment by weeks. Accurate coding isn’t just about compliance; it’s about speed.
What are some Best Practices for Dental Billing?
To maintain a 98% clean claim rate in the current landscape, you need a playbook that goes beyond just “sending the bill.” Here are the non-negotiables:
-
Shift from Denial Management to Denial Prevention: Don’t wait for the rejection. Use “claim scrubbing” technology to catch missing X-rays or mismatched birthdates before the claim leaves your software.
-
Verify or Vanish: Perform real-time eligibility checks 48 hours before the appointment. In 2026, “active coverage” can change in a heartbeat due to employment shifts or plan maximums being hit at a specialist’s office.
-
The 24-Hour Rule: Claims should be submitted within 24 hours of service. The longer a claim sits on your local server, the higher the chance of it becoming “stuck” in a backlog.
-
Embrace Medical Integration: Don’t let dental maximums limit your care. If you are treating trauma, sleep apnea, or systemic-linked oral infections, learn to bill medical insurance. It’s a six-figure growth opportunity most practices ignore.
How Can Guardian Dental Billing Help?
You didn’t go to dental school to spend four hours a day arguing with insurance adjusters. At Guardian Dental Billing, we act as the protective shield for your practice’s financial health.
We don’t just “process claims”—we manage your entire Revenue Cycle. Here is how we expand your business:
-
Immediate Cash Flow Injection: Our first task is often “AR Cleanup.” We hunt down every dollar stuck in your 30, 60, and 90-day buckets, providing an immediate boost to your working capital.
-
Expertise Without the Overhead: Hiring and training a high-level biller in-house is expensive and risky. When you partner with us, you get a team of CDT experts, medical-cross-coding specialists, and denial-negotiation pros for a fraction of the cost of a full-time employee.
-
Strategic Growth Reporting: We don’t just give you numbers; we give you insights. We’ll show you which insurance plans are costing you money in “write-offs” and where you have untapped revenue opportunities in your existing patient base.
-
Seamless Scalability: Whether you are a solo practitioner or a growing DSO, our systems scale with you. We handle the paperwork so you can focus on the patient in the chair.
In 2026, the practices that thrive are the ones that treat their billing like a professional revenue department. Guardian Dental Billing is that department.
Frequently Asked Questions About Dental Billing
Why is my dental claim taking so long to process?